 |
–Bart-Jan Kullberg, MD
ABSTRACT
Although cryptococcosis is the most frequent, zygomycosis, candidiasis, and aspergillosis are the other opportunistic cerebral mycoses that occur in Europe. Zygomycosis is caused by molds found in soil, fruit, and decaying vegetation. Rhinocerebral zygomycosis is an aggressive and destructive infection that leads to necrosis and infarction spreading mostly from the nasal cavity. Because the infection is associated with diabetic ketoacidosis, treatment begins with correction of the acidosis, followed by surgery and antifungal agents. High doses are recommended.
Candida meningitis is a rare candidal infection of the central nervous system. Three distinct forms of this infection are chronic Candida meningitis, Candida meningitis in patients with acquired immune deficiency syndrome, and Candida meningitis in neurosurgery patients. The clinical course differs for each.
Cerebral aspergillosis is almost always the result of hematogenous dissemination of primary pulmonary aspergillosis, with more than 95% of cases seen in patients with leukemia, lymphoma, or a bone marrow transplant. Treatment methods include surgery and the use of antifungal agents. The most generally accepted approach to therapy with antifungal agents is to administer the highest possible dose. Although treatment with antifungal agents is associated with high failure rates, studies evaluating newer agents are showing better results.
(Advanced Studies in Medicine. 2003;3(1A):S10-S11)
|
The 4 opportunistic cerebral mycoses that occur in Europe are cryptococcosis, which is the most frequent, and the rarer zygomycosis, candidiasis, and aspergillosis. Whereas the clinical picture and treatment of cryptococcosis are well known, management of the rarer fungal infections of the brain and central nervous system is also clinically challenging.
Zygomycosis
Also known as mucormycosis, zygomycosis is caused by molds found in soil, fruit, and decaying vegetation. The most common route of infection is through the nose, although direct cutaneous transmission occurs occasionally.
Rhinocerebral zygomycosis is an aggressive and destructive infection that progresses rapidly and causes necrosis and infarction of bony structures in and near the nasal cavities. It typically presents mimicking bacterial sinusitis; may spread downward from the nasal cavity through the hard palate, where an oral ulcer may develop; and extends from the nasal cavities and sinuses either upward into the frontal lobe or to the orbit and temporal lobe. When the orbit is involved, there is often protrusion of the eyeball. Lesions should be evaluated by biopsy to determine the presence of molds.
Rhinocerebral zygomycosis should be suspected in diabetic patients with ketoacidosis who do not respond to antibiotic therapy. Patients undergoing hemodialysis who are treated with iron-chelating agents are also at risk for this infection. Treatment begins with correction of the underlying condition and is followed by surgery.
Because zygomycosis is intrinsically resistant to most antifungal agents, including itraconazole, fluconazole, voriconazole, and flucytosine, the preferred medical therapy is amphotericin B. Many physicians try to administer the highest possible dose. Although there have been no comparative trials evaluating the efficacy of high-dose lipid-associated amphotericin B therapy, clinical results with high doses have been fairly good. Recent studies of posaconazole demonstrate increased in vitro activity against zygomycosis, but clinical results are not yet available.
Candidiasis
Cerebral candidiasis is the result of hematogenously disseminated candidiasis. Brain abscesses are rare, with the reported overall incidence in patients with disseminated candidiasis ranging from below 1% to 2%1; however, various autopsy series have put the incidence at 7% to 17%. Those who are at highest risk for cerebral candidiasis are newborns and patients who are neutropenic.
The most usual candidal infection of the central nervous system is Candida meningitis, which has 3 forms: chronic Candida meningitis, Candida meningitis in patients with acquired immune deficiency syndrome (AIDS), and Candida meningitis in neurosurgery patients.
Chronic Candida meningitis is characterized by a headache that progresses over a period of weeks or even months and is associated with confusion, vomiting, stupor, hydrocephalus, and coma. Known risk factors are present in 75% of cases, and nuchal rigidity is present in 60%. Laboratory findings include low glucose levels and a white blood cell count of 200/µL to 500/µL (monocytes and polymorphic leukocytes) in the cerebrospinal fluid.
Candida meningitis in AIDS patients has a sub-acute course that usually runs for fewer than 4 weeks and is predominantly related to intravenous drug use. In AIDS patients, having low CD4 counts is not a risk factor for invasive or disseminated candidiasis, but most affected patients have additional risk factors, such as drug-induced neutropenia.
Risk factors for Candida meningitis in neurosurgery patients include long-term use of ventriculoperitoneal shunts and broad-spectrum antibiotics, and recent neurosurgery. Therapy consists of a combination of shunt removal and antifungal agents.
Aspergillosis
Cerebral aspergillosis is the most frequent of the opportunistic fungal infections of the central nervous system, and is almost always the result of hematogenous dissemination of primary hematogenous aspergillosis. More than 95% of cases are seen in patients with leukemia, lymphoma, or a bone marrow transplant2; cerebral aspergillosis is rarely seen in patients with AIDS.
Radiologic findings in patients with aspergillosis of the central nervous system may be more typical of brain infarction than of brain abscess. Recent studies have found that the galactomannan antigen enzyme-linked immunosorbent assay may be useful for early diagnosis.
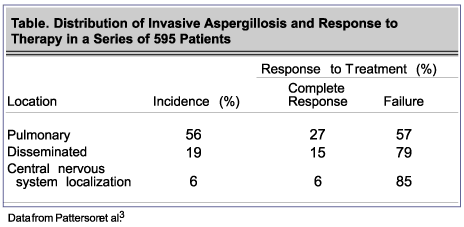
Treatment methods for aspergillosis include surgery, amphotericin B, lipid-associated amphotericin B, itraconazole, and newer antifungal agents, such as voriconazole or caspofungin. In general, treatment of invasive aspergillosis with antifungal agents has a high failure rate, as shown in the Table.3 Although the best approach regarding the use of antifungal agents has not yet been determined, the most generally accepted approach is to administer the highest possible dose of amphotericin B. Recent published data show that voriconazole is highly effective compared with amphotericin B for the treatment of invasive Aspergillus infection.4 Published data on the use of caspofungin in cerebral aspergillosis are not available.
REFERENCES
- Filler SG, Kullberg BJ. Deep-seated candidiasis. In: Calderone R, ed. Candida and Candidiasis. Washington, DC: American Society of Microbiology; 2001:341-348.
- Bodey G, Bueltman B, Duguid W, et al. Fungal infections in cancer patients: an international autopsy survey. Eur J Clin Microbiol Infect Dis. 1992;11:99-109.
- Patterson TF, Kirkpatrick WR, White M, et al. Invasive aspergillosis. Disease spectrum, treatment practices, and outcomes. Medicine. 2000;79:250-260.
- Herbrecht R, Denning DW, Patterson TF, et al. Voriconazole versus amphotericin B for primary therapy of invasive aspergillosis. N Engl J Med. 2002;347:408-415.
*Based on a presentation given by Dr Kullberg at the 12th European Congress of Clinical Microbiology and Infectious Diseases.
Address correspondence to: Bart-Jan Kullberg, MD, Department of Internal Medicine 541, University Hospital Nijmegen, Geert Grooteplein 8, Postbox 9101, 6500 HB Nijmegen, The Netherlands.
Volume 3, Number 1A - January 2003
This CME Expires on January 15, 2005; no tests will be accepted after this date.
This course is accredited by
Johns Hopkins University School of Medicine Advanced Studies in Medicine
|
 |

