Risk factors for IFI in patients receiving treatment for hematologic malignancies are closely linked with the degree of immune dysfunction and subsequent rate of recovery. A myriad of risk factors may coexist in any one patient. Dividing patients into risk categories – low, intermediate, high – is at best arbitrary. However, a number of risk factors have a definite link with a high incidence of IFI (Table 3).

| | Candidiasis | Aspergillosis
|
| Type of HSCT |
|
| (a) Autologous |  | 
|
| (b) Allogeneic – matched unrelated |  | 
|
| (c) Allogeneic – mismatched |  | 
|
|
| Cancers undergoing therapy |
|
| Lymphoma |  | 
|
| ALL |  | 
|
| AML |  | 
|
| Solid tumors |  |
|
|
| Total-body irradiation |  | 
|
|
| Mucosal injury |
|
| 1. During neutropenia |  |
|
| 2. Colonization with Candida species |  |
|
|
| Neutropenia |
|
| 0.1–0.5/mm3 <3 weeks |  | 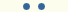
|
| <0.1/mm3 >3 weeks | 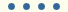 | 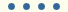
|
| <0.5/mm3 >5 weeks | 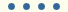 | 
|
|
| Corticosteroids >2 mg/kg/day >2 weeks |  | 
|
|
| Central venous catheter |  |
|
|
| Older age |  |
|
|
| Graft-versus-host disease |  | 
|
|
| Construction (eg, hospital) | | 
|
|
| Broad-spectrum antibiotics |  |
|
|
| CMV infection |  | 
|
|
HSCT=hematopoietic stem-cell transplant, ALL=acute lymphoblastic leukemia,
AML=acute myeloid leukemia, CMV=cytomegalovirus.
|
Neutropenia is one of the most important risk factors for IFI. Both the severity and duration of neutropenia define the degree of risk. Most infections occur when the circulating neutrophil count is <100/mm3 and neutropenia lasts for more than 3 weeks.
Degree of mucosal injury is an important risk factor for Candida infections.15,16 Different Candida species have varying capacities to penetrate the gut mucosa, explaining the association between C albicans or C tropicalis and systemic candidiasis in patients receiving conditioning regimens that cause extensive mucosal damage.17 Prior colonization is almost a prerequisite for invasive candidiasis, although nosocomial transmission of organisms from patient to patient, or from health-care workers or hospital environment to patient, occasionally occurs. Alteration of the gastrointestinal flora with broad-spectrum antibiotics allows commensal organisms to proliferate and increases the risk of IFI.15 Risk of IFI increases if more than one site, or heavy colonization at a single site, is found.18
It is well recognized that corticosteroid use increases infection rates. In the HSCT patient, the use of steroids after engraftment as prophylaxis for GVHD has been shown to increase the incidence of IFI 6-fold.19 Immunosuppressive agents such as fludarabine and cladrabine15 contribute to profound immunodeficiency and an increased risk of IFI. CMV infection, with its attendant leukopenia and gastrointestinal inflammation, potentiates infection with opportunistic pathogens, particularly in patients with active GVHD.10, 20,21 Finally, the universal use of central venous catheters is a potential source of infection.
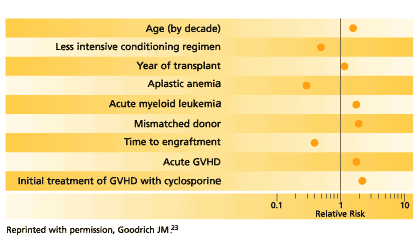
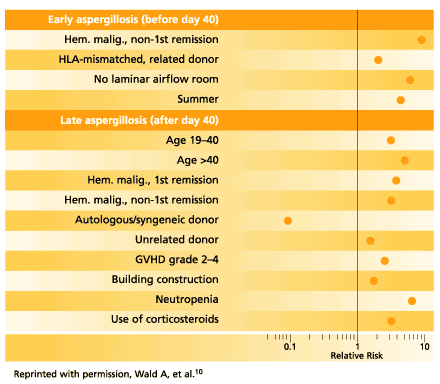
It is axiomatic that not all risk factors will be present at any one time and in any one patient.22 Multivariable analyses of case-control studies in a variety of cancer populations each reveal differing risk factors for fungemia.10,18,20,23 Relative risks for candidemia20 and aspergillosis10 in HSCT patients from one center are shown in Figures 3a and 3b.

Course Number: V035D
This CME Expires on July 1, 2005; no tests will be accepted after this date.
This course is accredited by
The University of Pittsburgh School of Medicine, Center for Continuing Education and The International Immunocompromised Host Society
|

