Treatment regimens for immunosuppression and chemotherapy have become standardized in recent years, thus facilitating the prediction of time to infection and type of infection. Exposure to fungal organisms can occur either in the community or in the hospital setting, and both recent and remote exposures are important in the development of invasive disease. Impaired host defenses can cause reactivation of dormant infection acquired some time previously, reinfection due to loss of immunity to a particular organism, or a primary infection. The timetable of infectious disease in organ-transplant recipients has been comprehensively documented (Fig 7) [44].
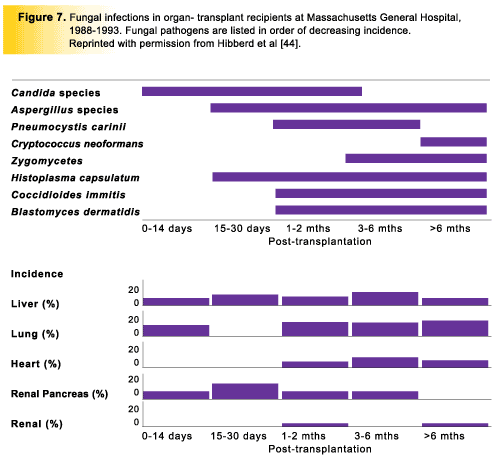 The early phase (within 1 month of transplantation) can be associated with infection in the patient before transplantation. Although actively infected patients rarely receive transplants, heavy colonization with agents such as Candida or Aspergillus may predispose patients to invasive infection when mucocutaneous barriers are disrupted. Further, fungal infection can be conveyed with the allograft, and rare cases of histoplasmosis and coccidioidomycosis have been reported. Infection can be nosocomially acquired during the perioperative period, primarily due to Candida species. More than 95% of infections in this early phase are the result of technical problems associated with the surgical procedure and postoperative management. Aspergillus species are notably absent.
The early phase (within 1 month of transplantation) can be associated with infection in the patient before transplantation. Although actively infected patients rarely receive transplants, heavy colonization with agents such as Candida or Aspergillus may predispose patients to invasive infection when mucocutaneous barriers are disrupted. Further, fungal infection can be conveyed with the allograft, and rare cases of histoplasmosis and coccidioidomycosis have been reported. Infection can be nosocomially acquired during the perioperative period, primarily due to Candida species. More than 95% of infections in this early phase are the result of technical problems associated with the surgical procedure and postoperative management. Aspergillus species are notably absent.
Up to 6 months after transplantation a high state of immunosuppression exists, and viral infections, particularly CMV, increase the chance of opportunistic infection. Protection of patients from environmental risks is of paramount importance.
Six months after transplantation patients with a successful allograft are at low risk of infection. However, patients with acute or chronic rejection who have required extensive immunosuppressive therapy and who are often infected with viruses are at increased risk of life-threatening infection.
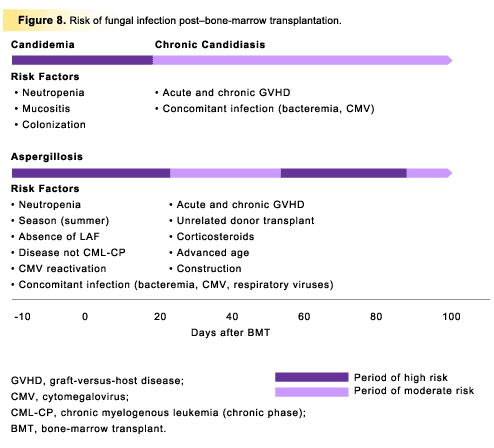
Periods of risk have also been documented [19, 27, 45] for BMT recipients (Fig 8). During the preengraftment period (days 0 to 30), prolonged profound neutropenia exists, and barrier protection is lost as a side effect of the conditioning regimens. Risk of infection is high; at most treatment centers, the median onset is 2 weeks after transplantation, with Candida and Aspergillus species the most commonly reported organisms. The postengraftment period(days 30 to 100) normally sees resolution of neutropenia and mucosal repair. However, during this period, chronic disseminated candidiasis can occur as the increasing neutrophil count engenders an inflammatory response to Candida seeded in the liver during the neutropenic period. Also, the presence of GVHD and immunosuppressive agents for treatment are significant risk factors affecting the severity and type of infection. During the late post-transplantation period (100 days and later), systemic infections are generally uncommon in the absence of chronic GVHD and associated organ damage, and oropharyngeal candidiasis is the most frequent fungal infection.
Course Number: V035B.043001
This CME Expires on July 1, 2003; no tests will be accepted after this date.
This course is accredited by
The University of Pittsburgh School of Medicine, Center for Continuing Education
|

